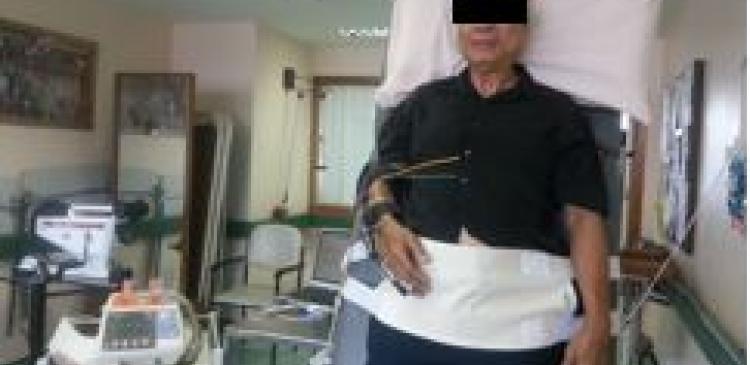
Functional reach is a measure of dynamic balance, and is performed by first obtaining the measurement on the metre rule at the position of the middle finger. The participant is then asked to reach out as far as possible without falling over, and the new measurement obtained. The distance between the first and second measurement is the functional reach.
Falls are common in the older population. The annual incidence of falls is nearly 30% in individuals 65 years and above and the number is expected to increase further as the population ages [1]. Falls in older people lead to physical disability, psychosocial problems, and deterioration in quality of life and reduced survival [2,3]. It often results in hospitalization and institutionalization with expensive medical costs [4]. Falls in the elderly are associated with numerous risk factors, e.g. physical limitation, gait and balance deficits, visual impairment, chronic medical illness, neurological disorders and postural hypotension (a condition linked to a drop in blood pressure withstanding)[5,6]. The study by a group of researchers from University of Malaya recruited older people who had at two falls or one fall with injury over the last 12 months. Their brain image were then compared with similar age people with no history of fall using MRI. A special advanced feature of MRI, Diffusion Tensor Imaging (DTI), was utilized in the study, allowing assessment of the white matter tracts within the brain.
The study assessed the whole brain microstructural integrity of major nerve tracts among the older individuals with a history of falls compared to non-fallers. 85 participants were evaluated clinically and using MRI of the brain [Figure1]. DTI was utilized to study the microstructural integrity of these white matter nerve tracts. Many clinical variables and risk factors known to be related to falls were also collected and analyzed using advanced statistical tests. It was proposed that there is potential synergistic relationship between blood pressure fluctuations with standing, balance disorders and structural brain abnormalities observed among fallers. This is the first study of its kind to utilize DTI for whole brain white tracts analysis while taking into account many contributing factors of fallers in an ageing multi-racial Asian population.
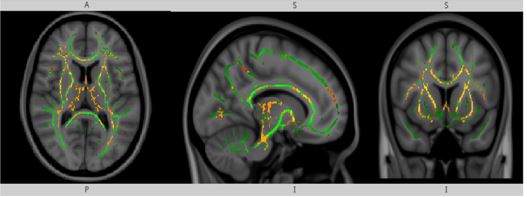
The researchers found several white matter nerve tracts that were significantly different between fallers and non-fallers, and the findings were published in Plos One [7]. Those tracts included the major nerve fibers that connecting the right and left cerebral hemisphere, as well as the cerebral and the lower brain (cerebellum, brainstem and spinal cord). The changes occur in several DTI metrics known as mean diffusivity (MD), axial diffusivity (AD) and radial diffusivity (RD). The researchers’ earlier works showed that an AD change not accompanied by FA changes is thought to represent widespread tissue damage, gross tissue loss and increased extracellular space [8]. Tract-based spatial statistics (TBBS) was used to analyze the DTI metrics. TBBS is an advanced computerized technique to overlay the fallers tracts over the normalized non-fallers tracts (known as TBBS skeleton), to highlight the nerve tracts which are significantly different between the two [Figure 2].
Besides the imaging features described above, there were other clinical and imaging variables which demonstrated significant differences between fallers and non-fallers such as the age, clinical parameters for gait and balance (functional-reach and time-up-and-go tests), white matter lesions volume (high signal focus on T2-weighted MRI sequence), hypertension, postural hypotension as well as fainting spells.
Using multivariate statistical analysis, the study showed that only presence of orthostatic hypotension, presence of hypertension, increased white matter lesions volume and decreased in functional-reach distance demonstrated statistical significant differences between fallers and non-fallers. No significant differences were found in the DTI metrics above when taking into account age and the four variables as covariates.
Therefore it was concluded that DTI metrics abnormality is not a singular factor that contributes independently to the fall outcomes. Instead, this novel finding importantly highlights the potentially synergistic effect between blood pressure changes, balance disorders and structural abnormalities of the brain in elderly falls. Nevertheless, the DTI aspect of this study helps to understand further the neurobiology underpinning movement and coordination disturbances in older population with falls. It may also serve as potential biomarkers in future falls intervention trials.
Acknowledgement
The UMMC and UMRIC brain research team consists of radiologists (Prof Norlisah Ramli, Assoc Prof Anushya Vijayananthan, Assoc Prof Khairul Azmi Abd Kadir, Dr Wong Yoke Queen); geriatrician (Prof Tan Maw Pin); medical physicist (Mr Tan Li Kuo) and research assistant (Ms Seow Pohchoo).
Contact
Prof Dr Norlisah Ramli
Department of Biomedical Imaging, Faculty of Medicine,
University of Malaya, 50603 Kuala Lumpur, Malaysia
E-mail: [email protected]
To highlight the white matter tracts affected in fallers we use the tract-based spatial statistics (TBSS). The white matter nerve tracts that demonstrated significant differences between the fallers and non-fallers are highlighted as follows with significance levels gradient (red < orange < yellow). TBSS baseline skeleton (green)