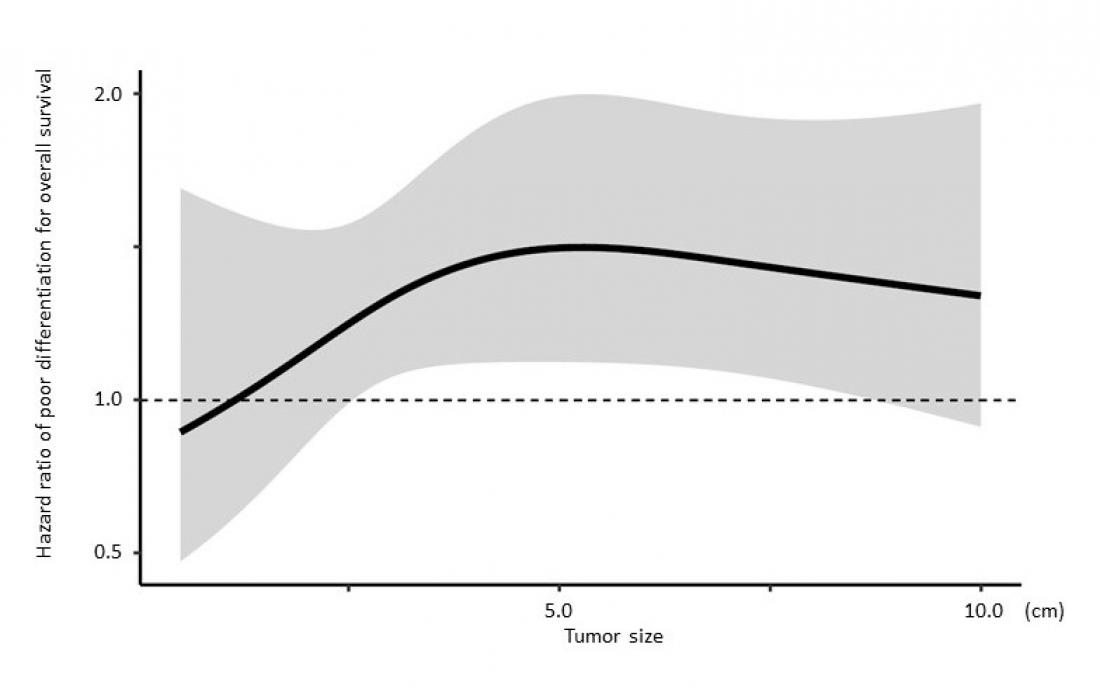
The horizontal axis shows tumor size, and the vertical axis shows the risk of poor prognosis. The risk of poor prognosis increases sharply for poorly differentiated hepatocellular carcinoma tumors ≥5 cm in size.
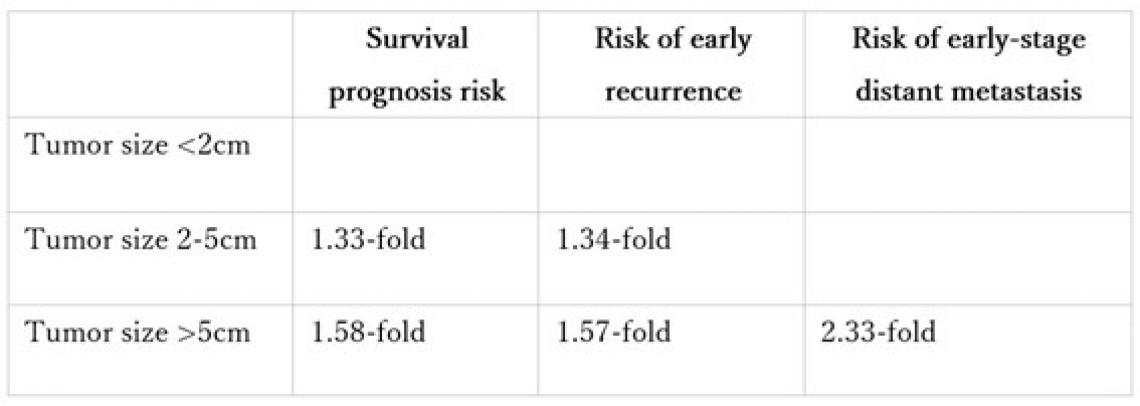
Poor prognostic risk of poorly differentiated hepatocellular carcinoma by grouping tumor size into <2 cm, 2-5 cm, and ≥5 cm.
OSAKA, Japan. Researchers at the Department of Hepato-Biliary-Pancreatic Surgery, Osaka City University Graduate School of Medicine have shown that the prognostic impact of hepatocellular carcinoma (HCC), the most common type of liver cancer, is dependent on tumor size.
The study findings, recently published in the journal Liver Cancer, fills in the need for an investigation into whether different sizes of poorly differentiated tumors affect rates of HCC early recurrence and prognosis.
“Poor differentiation (Por) speaks of the degree to which a cell stops looking and acting like a normal cell i.e. becomes a cancer cell” said first author of the study Dr. Hiroji Shinkawa. “In HCC, Por tumors refers to a cancer cells that are increasingly more disorganized under the microscope and grow and spread faster than other cancer cells.” By establishing a prognostic connection between Por tumors and overall survival, Dr. Shinkawa and his research team hope to improve medical intervention of HCC patients.
Using information dating back 30 years, Dr. Shinkawa and his team organized clinical data from 1,107 resected cases of HCC into 3 groups: tumors <2 cm, 2-5 cm, and ≥5 cm in size. To account for multiple variables like date of surgery, number and size of tumors, age, etc., the team used a multivariable Cox proportional hazards regression model to understand the association between HCC and patient survival time. Their results corroborated previous studies that Por tumors up to 2 cm in size have excellent long-term outcomes and they also found that Por tumors of 2-5 cm, and ≥5 cm in size had a 1.33- and 1.58-fold increased risk of poor prognosis, respectively.
“However, the key figure of this study,” states research advisor Dr. Shoji Kubo, “is that ≥5-sized tumors have a 2.33-fold risk of early extrahepatic recurrence.” Having a predictive marker of when a cancer may metastasize, of spread to other parts of the body, “raises clinically important concerns,” continues Dr. Kubo. In addition to increasing visits for patients with tumors ≥2 cm in size to check for local early recurrence of the cancer, both Dr. Shinkawa and Dr. Kubo agree that “physicians should perform an extrahepatic metastasis workup on patients with ≥5cm-sized tumors to prevent potential spreading of the disease.”
Lastly, clear predictors of early recurrence and early spreading of HCC will go hand in hand with postoperative drug therapies, such as molecular targeted drugs and immune checkpoint inhibitors, in improving the survival rate of the disease.
###
We are Osaka City University - the oldest research university in Osaka. With 9 undergraduate faculties and 11 graduate schools all dedicated to making urban life better, energy cleaner, and people healthier and happier, we have won numerous awards and have produced 2 Nobel laureates. For more information, please visit our website at https://www.osaka-cu.ac.jp/en