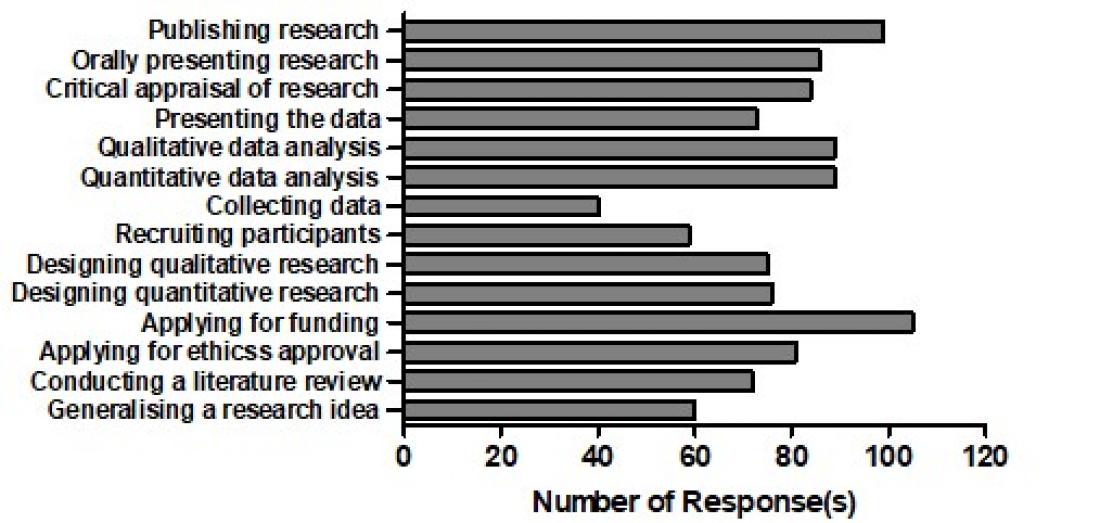
Fiq 1: Barriers of research skills
In sharp contrast with developed countries, the progress of health care disciplines across Asia has been slow and stagnated. A recent social-political phenomenon of dis-empowerment and dis-autonomy on their professional role has been observed in some countries. Many of the autonomous and independent departments of occupational therapy, physiotherapy and speech therapy have been restructured to be governed under a new governing regime by medical rehabilitation doctors. This act of occupational injustice has been facilitated because of Asia's entrenched medical model, and the consequences include declining job satisfaction among the health professionals, and creating a morbid environment of medical supremacy, according to a study published in JSM Health Education & Primary Health Care. More research are needed to scrutinise practices that are in line with the shrinking healthcare budgets and this calls for evidence-based, cost-effective direct interdisciplinary collaborations.
In the study, researchers in Malaysia argue that research activities and training needs for Health Care Professionals (HCPs) is fundamental for advancing the standards, quality and cost-effective deliveries of health care services. A study was conducted using universal sampling on three therapy disciplines - Occupational Therapy (OT), Speech therapy (ST) and Physiotherapy (PT). A total of 195 HCPs were approached to complete a 33-item survey questionnaire and out of 195 HCPs, 175 HCPs responded (a response rate of 89.7%). Speech Therapists reported the most active participation in research (85.7%), followed by Physiotherapists (18.1%) and Occupational Therapists (15.3%).
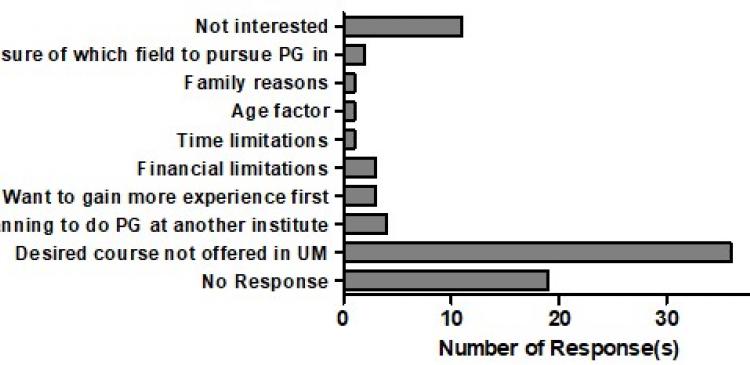
With research attitude, only 36.2 percent indicated a favourable attitude for research work, but majority (51.1%) are apathetic/neutral towards research activities. A survey on their research skills, showed that a high percentage had issues with research and almost 60 percent singled out 'fund-application' as a key barrier (Figure 1). However, some revealed that a current unfair ruling whereby HCPs were banned from independent research which do not have a rehabilitation doctor led as the Principal Investigator. Apart from socio-political barrier, almost all the respondents’ first professional education were at the very basic level of diploma-qualification (94.3%, n=165). Of this, only 13.7 percent (n=24) are currently pursuing their postgraduate studies. When asked if they would consider postgraduate studies, 50.9 percent (n=81) indicated that they were open towards continuing their studies. We explored reasons why they were not pursuing their postgraduate studies, 44.4 percent (n=36) said there were no discipline program even in their premier university for health sciences, and do not offer postgraduate programs for their desired courses, and 13.6 percent (n=11) revealed that they were not at all interested in pursuing further studies (Figure 2).
This survey found undesirable trend of research-interest in a group of young health professionals. With the current financial budget constraint, poor support system and an erosion of professional autonomy amongst HCPs in developing countries; an urgent calls for provision of more university-based education programs with timely policies to speed up progress, is clearly needed across Asia’s entrenched medical system governance. There is a dire need to remove the HCP's undergraduate diploma program still being conducted by the Ministry of Health, to the desirable standard of educational provision i.e. university-based degree and postgraduate opportunities under the Ministry of education and higher education.