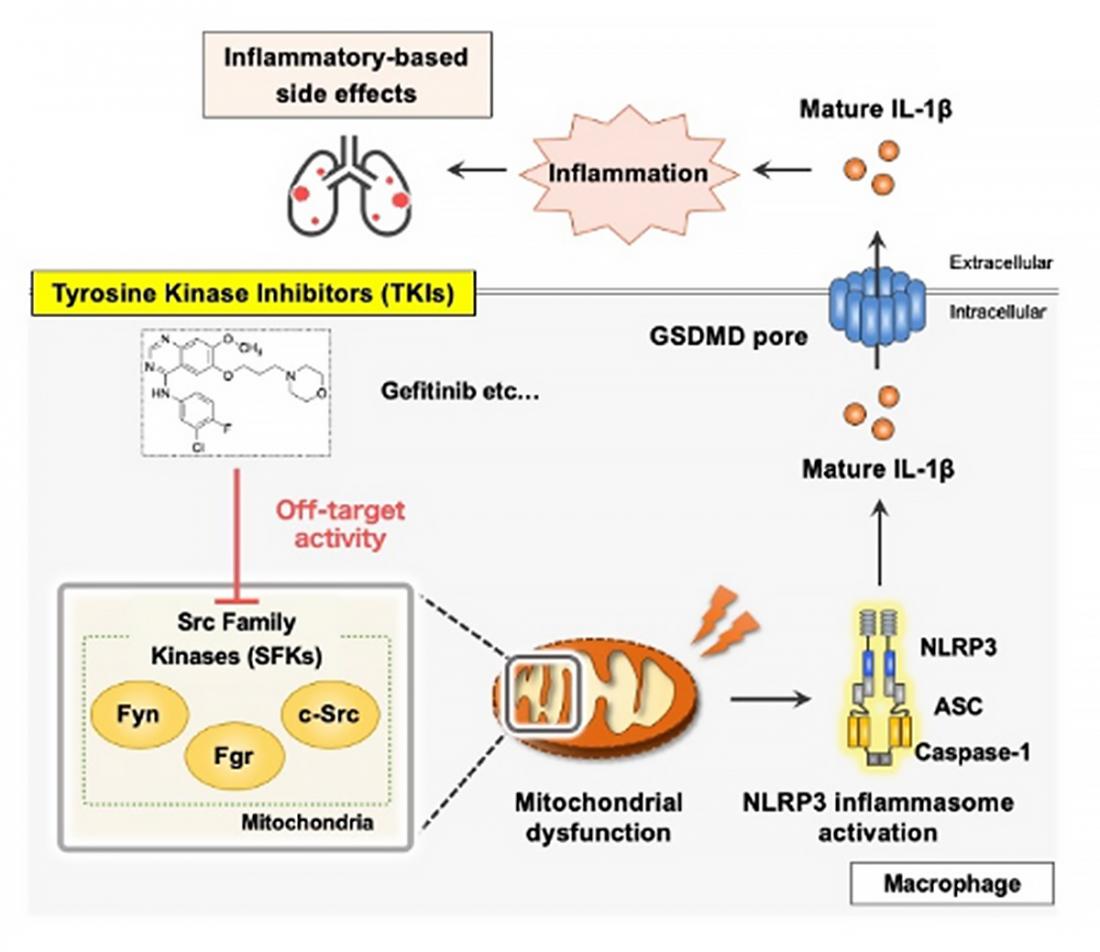
All TKIs we tested nonspecifically inhibit the kinase activity of the mitochondrial Src family kinases (mSFKs), which is responsible for the activation of the NLRP3 inflammasome. Therefore, the off-target activity against mSFKs appears to trigger the inflammatory-based side effects induced by TKIs.
Tyrosine kinase inhibitors are a type of targeted cancer medicine that can attack specific types of cancer cells and prevent them from multiplying. Although these inhibitors, called TKIs, can be very useful in fighting certain cancers, they also cause serious inflammatory side effects that limit their use. A Japanese research team has discovered the underlying mechanism that causes this inflammation.
"This study revealed the underlying mechanism by which the TKIs cause inflammation, and therefore provides the molecular basis that is essential to overcome the inflammatory-based side effects," said Atsushi Matsuzawa, a professor at the Laboratory of Health Chemistry, Graduate School of Pharmaceutical Sciences, Tohoku University.
The team's findings were published in The Journal of Immunology on February 6, 2023.
These TKIs are essential anticancer drugs. However, the use of TKIs frequently initiates inflammation in the body, such as the lung disease interstitial pneumonitis. From their earlier studies, the team had learned that a representative TKI called Gefitinib (GF) causes lung inflammation. GF is a helpful cancer medication used in treating certain breast, lung, and other cancers. It works by targeting the epidermal growth factor receptors. When the GF is used to treat the cancer, it can also cause inflammation in the patient's lungs, through the NLRP3 inflammasome. The NLRP3 inflammasome is part of the body's immune system and plays an important role in innate immunity. But when the NLRP3 inflammasome is improperly activated, it can contribute to the development of a wide range of inflammatory diseases.
Until now, scientists have not fully understood why the NLRP3 inflammasome is activated, but the evidence seems to point to mitochondrial dysfunction. When mitochondria are healthy, they work like batteries, producing energy in the body's cells. Mitochondrial dysfunction happens when the mitochondria do not work as they should because of disease. In their earlier study, the team learned that the GF activated the NLRP3 inflammasome through mitochondrial damage that led to the interstitial pneumonitis in patients. However, they had not understood how GF initiates the mitochondrial damage and whether or not other TKIs also shared this mechanism.
To conduct their study, the team looked at the tyrosine kinases, those enzymes that work as a kind of "on" and "off" switch in many of the cells' functions. They specifically studied the Src family kinases, called SFKs. The SFKs are nonreceptor tyrosine kinases that regulate many cell processes. There are 11 types of SFKs in the human genome. Some of these SFKs are in the mitochondria and they play an essential role in the function of the mitochondria. The team found that all the TKIs they tested inhibit the kinase activity of the SKFs in the mitochondria which is responsible for the NLRP3 inflammasome.
The team's comprehensive analysis of the TKIs they tested revealed that these TKIs act as powerful agonists. In addition, the team observed off-target activity that could contribute to the side effects. "As an important finding, all TKIs we tested share a common off-target activity against the mitochondrial SFKs. Therefore, blocking the access of TKIs to mitochondria is a good way to prevent the inflammation," said Matsuzawa. They also noted that the other TKIs that do not affect the activity of the mitochondrial SFKs may overcome the inflammatory-based side effects. As another approach, when effective inhibitors of the NLRP3 inflammasome are developed, administering the TKIs at the same time as the NLRP3 inhibitors can counteract the side effects. The team's results provide insight into both the biological and the clinical significance of the NLRP3 inflammasome and the SFKs.
Looking ahead, the team's next step is to propose a new approach to avoid the inflammatory-based side effects of TKIs. They hope to lead in the development of new TKIs that do not initiate inflammation.
The research team includes Yuto Sekiguchi, Saya Takano, Takuya Noguchi, Tomohiro Kagi, Ryuto Komatsu, Maoko Tan, Yusuke Hirata, and Atsushi Matsuzawa from the Laboratory of Health Chemistry, Graduate School of Pharmaceutical Sciences, Tohoku University, Japan.