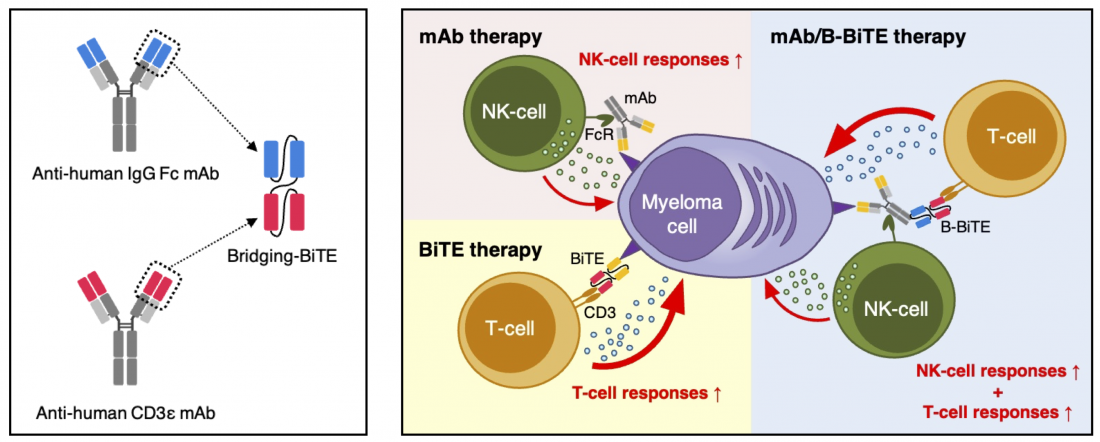
A monoclonal antibody can activate human NK cells, and a BiTE can stimulate human T cells against myeloma cells, separately. In contrast, the B-BiTE possesses two single chain variable fragments specific for the Fc region of the human IgG and human CD3 molecule. As a result, an mAb/B-BiTE complex safely and effectively targeted myeloma cells and other tumor cells via dual-lymphoid activation mediated by human T cells as well as NK cells.
Multiple myeloma still appears to be an incurable hematological malignancy. One of the reasons is that myeloma cells can be heterogenous and acquire resistance after anti-myeloma treatment. Immunotherapy is an attractive strategy to target myeloma cells with drug resistance. The next-generation modality which can safely and effectively strengthen immunotherapeutic effects while overcoming the characteristics of myeloma cells is now desirable in order to break through these obstacles.
In this study, we have developed a new modality, referred to as Bridging-Bispecific T-cell Engager (B-BiTE). B-BiTE bound to the Fc region of human immunoglobulin G monoclonal antibody (mAb) and human CD3 molecule expressed by T cells. When B-BiTE was applied to Daratumumab (Dar) specific for CD38 and Elotuzumab (Elo) reactive for SLAMF7, which are major clinical mAbs for the treatment of myeloma, human T cells as well as NK cells successfully and safely activated for a panel of different myeloma cells in the presence of Dar/B-BiTE or Elo/B-BiTE, resulting in dual-lymphoid activation. Moreover, anti-myeloma effects mediated by an mAb/B-BiTE complex were enhanced as compared to those in the presence of mAb alone. Importantly, using an in vivo myeloma model, we have shown that sequential immunotherapy using two different B-BiTE-based bispecifics, Dar/B-BiTE followed by Elo/B-BiTE, appeared to circumvent antigen escape by myeloma cells, and sufficiently induced deep and durable anti-myeloma responses relative to those induced by mAb/B-BiTE monotherapy or sequential therapy with two mAbs without B-BiTE.
Based on these findings, clinically available antibodies armed with B-BiTE have the potential to augment anti-myeloma effects. Furthermore, this approach would facilitate the easy and rapid preparation of B-BiTE-based bispecifics using a variety of clinical mAbs for the treatment of not only myeloma but also other refractory malignancies.